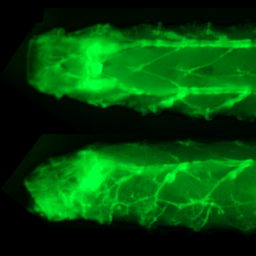
Driver mutations in major lung cancer oncogenes can be analyzed in Drosophila models
Main Article Content
Abstract
Lung cancer remains the leading cause of cancer-associated mortality. Despite recent promising achievements, the overall prognosis remains very poor. In order to integrate the advantages of adapted, transgenic animal models with a high-throughput procedure on the one hand and compliance with the 3R principles on the other hand, we have established and evaluated appropriate Drosophila models. To achieve this goal, we ectopically expressed oncogenes representing the most important driver mutations exclusively in the airway system. These oncogenes were either the human oncogenes or the corresponding Drosophila orthologs. We concentrated on two complementary read-out systems, 1) early larval lethality and 2) quantification of concurrently expressed GFP as a proxy for tumor mass. We could show that ectopic expression of EgfrCA, RasV12, Raf, Rolled (MAPK), PI3K92E, Alk, Akt and Arm can induce early lethality. Thus, they can be used in a straight-forward high-throughput screening approach and can replace mouse models to a considerable extent. Moreover, we could also show that measurement of tumor mass by a concurrently expressed marker (GFP) can be used to detect positive treatment results. Our results show that our Drosophila system provides a superb in vivo invertebrate screening system amenable to high-throughput approaches and thus effectively complements the toolbox for the development of novel anti-lung cancer treatments, while complying with the 3R principles.
Article Details

This work is licensed under a Creative Commons Attribution 4.0 International License.
Articles are distributed under the terms of the Creative Commons Attribution 4.0 International license (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution and reproduction in any medium, provided the original work is appropriately cited (CC-BY). Copyright on any article in ALTEX is retained by the author(s).
Adachi, Y., Yanagimura, N., Suzuki, C. et al. (2020). Reduced doses of dabrafenib and trametinib combination therapy for BRAF V600E-mutant non-small cell lung cancer prevent rhabdomyolysis and maintain tumor shrinkage: A case report. BMC Cancer 20, 156. doi:10.1186/s12885-020-6626-9
Andrew, D. J. and Ewald, A. J. (2010). Morphogenesis of epithelial tubes: Insights into tube formation, elongation, and elaboration. Dev Biol 341, 34-55. doi:10.1016/j.ydbio.2009.09.024
Bangi, E., Murgia, C., Teague, A. G. et al. (2016). Functional exploration of colorectal cancer genomes using Drosophila. Nat Commun 7, 13615. doi:10.1038/ncomms13615
Bangi, E., Ang, C., Smibert, P. et al. (2019). A personalized platform identifies trametinib plus zoledronate for a patient with KRAS-mutant metastatic colorectal cancer. Sci Adv 5, eaav6528. doi:10.1126/sciadv.aav6528
Behr, M. (2010). Molecular aspects of respiratory and vascular tube development. Respir Physiol Neurobiol 173, Suppl, S33-36. doi:10.1016/j.resp.2010.04.011
Blakemore, C., MaCarthur Clark, J., Nevalainen, T. et al. (2012). Implementing the 3Rs in neuroscience research: A reasoned approach. Neuron 75, 948-950. doi:10.1016/j.neuron.2012.09.001
Bossen, J., Uliczka, K., Steen, L. et al. (2019). An EGFR-induced Drosophila lung tumor model identifies alternative combination treatments. Mol Cancer Ther 18, 1659-1668. doi:10.1158/1535-7163.MCT-19-0168
Brand, A. H. and Perrimon, N. (1993). Targeted gene expression as a means of altering cell fates and generating dominant phenotypes. Development 118, 401-415.
Das, T. and Cagan, R. (2010). Drosophila as a novel therapeutic discovery tool for thyroid cancer. Thyroid 20, 689-695. doi:10.1089/thy.2010.1637
Ding, L., Getz, G., Wheeler, D. A. et al. (2008). Somatic mutations affect key pathways in lung adenocarcinoma. Nature 455, 1069-1075. doi:10.1038/nature07423
Gateff, E. (1978). Malignant neoplasms of genetic origin in Drosophila melanogaster. Science 200, 1448-1459. doi:10.1126/science.96525
Gervais, L. and Casanova, J. (2011). The Drosophila homologue of SRF acts as a boosting mechanism to sustain FGF-induced terminal branching in the tracheal system. Development 138, 1269-1274. doi:10.1242/dev.059188
Ghabrial, A., Luschnig, S., Metzstein, M. M. et al. (2003). Branching morphogenesis of the Drosophila tracheal system. Annu Rev Cell Dev Biol 19, 623-647. doi:10.1146/annurev.cellbio.19.031403.160043
Gonzalez, C. (2013). Drosophila melanogaster: A model and a tool to investigate malignancy and identify new therapeutics. Nat Rev Cancer 13, 172-183. doi:10.1038/nrc3461
Graham, M. L. and Prescott, M. J. (2015). The multifactorial role of the 3Rs in shifting the harm-benefit analysis in animal models of disease. Eur J Pharmacol 759, 19-29. doi:10.1016/j.ejphar.2015.03.040
Harrison, D. A., Binari, R., Nahreini, T. S. et al. (1995). Activation of a Drosophila Janus kinase (JAK) causes hematopoietic neoplasia and developmental defects. EMBO J 14, 2857-2865. doi:10.1002/j.1460-2075.1995.tb07285.x
Kallsen, K., Zehethofer, N., Abdelsadik, A. et al. (2015). ORMDL deregulation increases stress responses and modulates repair pathways in Drosophila airways. J Allergy Clin Immunol 136, 1105-1108. doi:10.1016/j.jaci.2015.04.009
Kandoth, C., McLellan, M. D., Vandin, F. et al. (2013). Mutational landscape and significance across 12 major cancer types. Nature 502, 333-339. doi:10.1038/nature12634
Kretlow, A., Butzke, D., Goetz, M. E. et al. (2010). Implementation and enforcement of the 3Rs principle in the field of transgenic animals used for scientific purposes. Report and recommendations of the BfR expert workshop, May 18-20, 2009, Berlin, Germany. ALTEX 27, 117-134. doi:10.14573/altex.2010.2.117
Kwon, M. C. and Berns, A. (2013). Mouse models for lung cancer. Mol Oncol 7, 165-177. doi:10.1016/j.molonc.2013.02.010
Levine, B. D. and Cagan, R. L. (2016). Drosophila lung cancer models identify trametinib plus statin as candidate therapeutic. Cell Rep 14, 1477-1487. doi:10.1016/j.celrep.2015.12.105
Levinson, S. and Cagan, R. L. (2016). Drosophila cancer models identify functional differences between ret fusions. Cell Rep 16, 3052-3061. doi:10.1016/j.celrep.2016.08.019
Luo, S. Y. and Lam, D. C. (2013). Oncogenic driver mutations in lung cancer. Transl Respir Med 1, 6. doi:10.1186/2213-0802-1-6
Markstein, M., Dettorre, S., Cho, J. et al. (2014). Systematic screen of chemotherapeutics in Drosophila stem cell tumors. Proc Natl Acad Sci U S A 111, 4530-4535. doi:10.1073/pnas.1401160111
Meijering, E., Jacob, M., Sarria, J.-C. F. et al. (2004). Design and validation of a tool for neurite tracing and analysis in fluorescence microscopy images. Cytometry Part A 58, 167-176. doi:10.1002/cyto.a.20022
Olsson, I. A. S., Franco, N. H., Weary, D. M. et al. (2012). The 3Rs principle – Mind the ethical gap. Proceedings of the 8th World Congress on Alternatives and Animal Use in the Life Sciences, Montreal, 2011. ALTEX Proc 1, 333-336. https://proceedings.altex.org/?2012-01
Paez, J. G., Janne, P. A., Lee, J. C. et al. (2004). EGFR mutations in lung cancer: Correlation with clinical response to gefitinib therapy. Science 304, 1497-1500. doi:10.1126/science.1099314
Roeder, T., Isermann, K. and Kabesch, M. (2009). Drosophila in asthma research. Am J Respir Crit Care Med 179, 979-983. doi:10.1164/rccm.200811-1777PP
Roeder, T., Isermann, K., Kallsen, K. et al. (2012). A Drosophila asthma model – What the fly tells us about inflammatory diseases of the lung. Adv Exp Med Biol 710, 37-47. doi:10.1007/978-1-4419-5638-5_5
Rosell, R., Carcereny, E., Gervais, R. et al. (2012). Erlotinib versus standard chemotherapy as first-line treatment for European patients with advanced EGFR mutation-positive non-small-cell lung cancer (EURTAC): A multicentre, open-label, randomised phase 3 trial. Lancet Oncol 13, 239-246. doi:10.1016/S1470-2045(11)70393-X
Rotow, J. and Bivona, T. G. (2017). Understanding and targeting resistance mechanisms in NSCLC. Nat Rev Cancer 17, 637-658. doi:10.1038/nrc.2017.84
Ruehle, H. (1932). Das larvale Tracheensystem von Drosophila melanogaster Meigen und seine Variabilität [Article in German]. Zeitschrift für wissenschaftliche Zoologie 141, 159-245.
Sharma, S. V., Bell, D. W., Settleman, J. et al. (2007). Epidermal growth factor receptor mutations in lung cancer. Nat Rev Cancer 7, 169-181. doi:10.1038/nrc2088
Siegelin, M. D. and Borczuk, A. C. (2014). Epidermal growth factor receptor mutations in lung adenocarcinoma. Lab Invest 94, 129-137. doi:10.1038/labinvest.2013.147
Stewart, B. W. and Wild, C. P. (eds.) (2014). World Cancer Report 2014. International Agency for Research on Cancer. WHO Press.
Travis, W. D., Brambilla, E., Nicholson, A. G. et al. (2015). The 2015 world health organization classification of lung tumors: Impact of genetic, clinical and radiologic advances since the 2004 classification. J Thorac Oncol 10, 1243-1260. doi:10.1097/JTO.0000000000000630
Wagner, C., Isermann, K., Fehrenbach, H. et al. (2008). Molecular architecture of the fruit fly’s airway epithelial immune system. BMC Genomics 9, 446. doi:10.1186/1471-2164-9-446
Wagner, C., Isermann, K. and Roeder, T. (2009). Infection induces a survival program and local remodeling in the airway epithelium of the fly. FASEB J 23, 2045-2054. doi:10.1096/fj.08-114223
Whitten, J. (1957). The post-embryonic development of the tracheal system in Drosophila melanogaster. Q J Microsc Sci 98, 123-150.
Willoughby, L. F., Schlosser, T., Manning, S. A. et al. (2013). An in vivo large-scale chemical screening platform using Drosophila for anti-cancer drug discovery. Dis Model Mech 6, 521-529. doi:10.1242/dmm.009985