Clean bioprinting - Fabrication of 3D organ models devoid of animal components
Main Article Content
Abstract
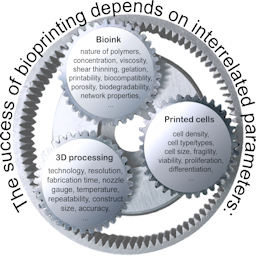
Bioprinting is a rapidly developing technology that enables the exact positioning of living cells embedded in bio-materials in precise spatial arrangements to fabricate engineered tissues and organs. While the ultimate goal of bioprinting approaches is to produce organs for transplantation purposes, bioprinted organ models also hold great potential for research purposes to serve as alternatives to animal experiments. By using human cells, humanized organ models can be generated that may produce more relevant results for human (patho-)physiology than animal models. However, standard bioprinting procedures currently use numerous hidden animal components. Virtually all studies published in the field to date make use of cells grown in media with fetal bovine serum (FBS). In addition, Matrigel, the extracellular matrix (ECM) harvested from Engelbreth-Holm-Swarm sarcoma grown in mice, is widely employed to cultivate stem cells and 3D organ models. Finally, most bioinks currently in use contain gelatin or comparable animal components to improve cell viability and adhesion. The present review will give an introduction to the potential of bioprinting to fabricate 3D models that may be substituted for animal experiments and will go on to describe strategies to replace animal components currently included in standard procedures of bioprinting. These approaches comprise the adaptation of cells to FBS-free media, the use of bioinks composed of synthetic or plant material, and the replacement of animal ingredients by materials of human origin. We propose denoting bioprinting strategies devoid of animal components as clean bioprinting.
Article Details

This work is licensed under a Creative Commons Attribution 4.0 International License.
Articles are distributed under the terms of the Creative Commons Attribution 4.0 International license (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution and reproduction in any medium, provided the original work is appropriately cited (CC-BY). Copyright on any article in ALTEX is retained by the author(s).
Abasalizadeh, F., Moghaddam, S. V., Alizadeh, E. et al. (2020). Alginate-based hydrogels as drug delivery vehicles in cancer treatment and their applications in wound dressing and 3D bioprinting. J Biol Eng 14, 8. doi:10.1186/s13036-020-0227-7
Aisenbrey, E. A. and Murphy, W. L. (2020). Synthetic alternatives to Matrigel. Nat Rev Mater 5, 539-551. doi:10.1038/s41578-020-0199-8
Anderson, N. L., Polanski, M., Pieper, R. et al. (2004). The human plasma proteome: A nonredundant list developed by combination of four separate sources. Mol Cell Proteomics 3, 311-326. doi:10.1074/mcp.M300127-MCP200
Axpe, E. and Oyen, M. L. (2016). Applications of alginate-based bioinks in 3D bioprinting. Int J Mol Sci 17, 1976. doi:10.3390/ijms17121976
Baker, M. (2016). 1,500 scientists lift the lid on reproducibility. Nature 533, 452-454. doi:10.1038/533452a
Bejleri, D., Streeter, B. W., Nachlas, A. L. Y. et al. (2018). A bioprinted cardiac patch composed of cardiac-specific extracellular matrix and progenitor cells for heart repair. Adv Healthc Mater 7, e1800672. doi:10.1002/adhm.201800672
Benton, G., Arnaoutova, I., George, J. et al. (2014). Matrigel: From discovery and ECM mimicry to assays and models for cancer research. Adv Drug Deliv Rev 79-80, 3-18. doi:10.1016/j.addr.2014.06.005
Berg, J., Zscheppang, K., Fatykhova, D. et al. (2017). Tyk2 as a target for immune regulation in human viral/bacterial pneumonia. Eur Respir J 50, 1601953. doi:10.1183/13993003.01953-2016
Berg, J., Hiller, T., Kissner, M. S. et al. (2018). Optimization of cell-laden bioinks for 3D bioprinting and efficient infection with influenza A virus. Sci Rep 8, 13877. doi:10.1038/s41598-018-31880-x
Bouvier, N. M. and Lowen, A. C. (2010). Animal models for influenza virus pathogenesis and transmission. Viruses 2, 1530-1563. doi:10.3390/v20801530
Boyd-Moss, M., Fox, K., Brandt, M. et al. (2017). Bioprinting and biofabrication with peptide and protein biomaterials. Adv Exp Med Biol 1030, 95-129. doi:10.1007/978-3-319-66095-0_5
Braam, S. R., Zeinstra, L., Litjens, S. et al. (2008). Recombinant vitronectin is a functionally defined substrate that supports human embryonic stem cell self-renewal via alphavbeta5 integrin. Stem Cells 26, 2257-2265. doi:10.1634/stemcells.2008-0291
Cakarova, L., Marsh, L. M., Wilhelm, J. et al. (2009). Macrophage tumor necrosis factor-alpha induces epithelial expression of granulocyte-macrophage colony-stimulating factor: Impact on alveolar epithelial repair. Am J Respir Crit Care Med 180, 521-532. doi:10.1164/rccm.200812-1837OC
Chen, Y., Stevens, B., Chang, J. et al. (2008). NS21: Re-defined and modified supplement B27 for neuronal cultures. J Neurosci Methods 171, 239-247. doi:10.1016/j.jneumeth.2008.03.013
Choudhury, D., Tun, H. W., Wang, T. et al. (2018). Organ-derived decellularized extracellular matrix: A game changer for bioink manufacturing? Trends Biotechnol 36, 787-805. doi:10.1016/j.tibtech.2018.03.003
Confino, C., Perez-Amodio, S., Semino, C. E. et al. (2019). Development of a self-assembled peptide/methylcellulose-base bioink for 3D bioprinting. Macromol Mater Eng 304, 1900353.
Crook, J. M. (ed.) (2020). 3D Bioprinting: Principles and Protocols. Totowa, NJ, USA: Humana Press.
Cui, X., Breitenkamp, K., Finn, M. G. et al. (2012). Direct human cartilage repair using three-dimensional bioprinting technology. Tissue Eng Part A 18, 1304-1312. doi:10.1089/ten.TEA.2011.0543
Daly, A. C., Critchley, S. E., Rencsok, E. M. et al. (2016a). A comparison of different bioinks for 3D bioprinting of fibrocartilage and hyaline cartilage. Biofabrication 8, 045002. doi:10.1088/1758-5090/8/4/045002
Daly, A. C., Cunniffe, G. M., Sathy, B. N. et al. (2016b). 3D bioprinting of developmentally inspired templates for whole bone organ engineering. Adv Healthc Mater 5, 2353-2362. doi:10.1002/adhm.201600182
Dasgupta, Q. and Black, L. D., 3rd (2019). A FRESH SLATE for 3D bioprinting. Science 365, 446-447. doi:10.1126/science.aay0478
Davison-Kotler, E., Marshall, W. S. and Garcia-Gareta, E. (2019). Sources of collagen for biomaterials in skin wound healing. Bioengineering (Basel) 6, 56. doi:10.3390/bioengineering6030056
de Melo, B. A. G., Jodat, Y. A., Cruz, E. M. et al. (2020). Strategies to use fibrinogen as bioink for 3D bioprinting fibrin-based soft and hard tissues. Acta Biomater 117, 60-76. doi:10.1016/j.actbio.2020.09.024
Dellambra, E., Odorisio, T., D’Arcangelo, D. et al. (2019). Non-animal models in dermatological research. ALTEX 36, 177-202. doi:10.14573/altex.1808022
Derr, K., Zou, J., Luo, K. et al. (2019). Fully three-dimensional bioprinted skin equivalent constructs with validated morphology and barrier function. Tissue Eng Part C Methods 25, 334-343. doi:10.1089/ten.TEC.2018.0318
Domalik-Pyzik, P., Chłopek, J. and Pielichowska, K. (2019). Chitosan-based hydrogels: Preparation, properties, and applications. In M. Mondal (ed.), Cellulose-Based Superabsorbent Hydrogels. Polymers and Polymeric Composites: A Reference Series (1665-1693). Cham, Switzerland: Springer. doi:10.1007/978-3-319-77830-3_55
Duan, B., Kapetanovic, E., Hockaday, L. A. et al. (2014). Three-dimensional printed trileaflet valve conduits using biological hydrogels and human valve interstitial cells. Acta Biomater 10, 1836-1846. doi:10.1016/j.actbio.2013.12.005
Eo, J. S., Soo, H. J., Jong-Ock, S. et al. (2017). Extracellular matrix and 3D printing. Curr Trends Biomedical Eng Biosci 2, 55596. doi:10.19080/ctbeb.2017.02.555596
Fan, R., Piou, M., Darling, E. et al. (2016). Bio-printing cell-laden Matrigel-agarose constructs. J Biomater Appl 31, 684-692. doi:10.1177/0885328216669238
Fan, Y., Zhang, F. and Tzanakakis, E. S. (2017). Engineering xeno-free microcarriers with recombinant vitronectin, albumin and UV irradiation for human pluripotent stem cell bioprocessing. ACS Biomater Sci Eng 3, 1510-1518. doi:10.1021/acsbiomaterials.6b00253
Fay, C. D. (2020). Computer-aided design and manufacturing (CAD/CAM) for bioprinting. Methods Mol Biol 2140, 27-41. doi:10.1007/978-1-0716-0520-2_3
Francis, G. L. (2010). Albumin and mammalian cell culture: Implications for biotechnology applications. Cytotechnology 62, 1-16. doi:10.1007/s10616-010-9263-3
Ghormade, V., Pathan, E. K. and Deshpande, M. V. (2017). Can fungi compete with marine sources for chitosan production? Int J Biol Macromol 104, 1415-1421. doi:10.1016/j.ijbiomac.2017.01.112
Gonzalez Hernandez, Y. and Fischer, R. W. (2007). Serum-free culturing of mammalian cells – Adaptation to and cryopreservation in fully defined media. ALTEX 24, 110-116. doi:10.14573/altex.2007.2.110
Gopinathan, J. and Noh, I. (2018). Recent trends in bioinks for 3D printing. Biomater Res 22, 11. doi:10.1186/s40824-018-0122-1
Grigoryan, B., Paulsen, S. J., Corbett, D. C. et al. (2019). Multivascular networks and functional intravascular topologies within biocompatible hydrogels. Science 364, 458-464. doi:10.1126/science.aav9750
Grix, T., Ruppelt, A., Thomas, A. et al. (2018). Bioprinting perfusion-enabled liver equivalents for advanced organ-on-a-chip applications. Genes (Basel) 9, 176. doi:10.3390/genes9040176
Groll, J., Burdick, J. A., Cho, D. W. et al. (2018). A definition of bioinks and their distinction from biomaterial inks. Biofabrication 11, 013001. doi:10.1088/1758-5090/aaec52
Gstraunthaler, G. (2003). Alternatives to the use of fetal bovine serum: Serum-free cell culture. ALTEX 20, 275-281. https://www.altex.org/index.php/altex/article/view/1012
Gstraunthaler, G., Lindl, T. and van der Valk, J. (2013). A plea to reduce or replace fetal bovine serum in cell culture media. Cytotechnology 65, 791-793. doi:10.1007/s10616-013-9633-8
Gungor-Ozkerim, P. S., Inci, I., Zhang, Y. S. et al. (2018). Bioinks for 3D bioprinting: An overview. Biomater Sci 6, 915-946. doi:10.1039/c7bm00765e
Hackethal, J., Hofer, A., Hennerbichler, S. et al. (2019). A comparison of enzymatic and non-enzymatic strategies to isolate extracellular matrix (ECM) proteins from human placenta and liposuction fat. ALTEX Proc 8, 65. https://proceedings.altex.org/?2019-01
Hafezi, F., Scoutaris, N., Douroumis, D. et al. (2019). 3D printed chitosan dressing crosslinked with genipin for potential healing of chronic wounds. Int J Pharm 560, 406-415. doi:10.1016/j.ijpharm.2019.02.020
Han, S., Kim, S., Chen, Z. et al. (2020). 3D bioprinted vascularized tumour for drug testing. Int J Mol Sci 21, 2993. doi:10.3390/ijms21082993
Heinrich, M. A., Liu, W. J., Jimenez, A. et al. (2019). 3D bioprinting: From benches to translational applications. Small 15, e1805510. doi:10.1002/smll.201805510
Hiller, T., Berg, J., Elomaa, L. et al. (2018). Generation of a 3D liver model comprising human extracellular matrix in an alginate/gelatin-based bioink by extrusion bioprinting for infection and transduction studies. Int J Mol Sci 19, 3129. doi:10.3390/ijms19103129
Homan, K. A., Kolesky, D. B., Skylar-Scott, M. A. et al. (2016). Bioprinting of 3D convoluted renal proximal tubules on perfusable chips. Sci Rep 6, 34845. doi:10.1038/srep34845
Horvath, L., Umehara, Y., Jud, C. et al. (2015). Engineering an in vitro air-blood barrier by 3D bioprinting. Sci Rep 5, 7974. doi:10.1038/srep07974
Hoshiba, T. (2017). Cultured cell-derived decellularized matrices: A review towards the next decade. J Mater Chem B 5, 4322-4331. doi:10.1039/c7tb00074j
Hospodiuk, M., Dey, M., Sosnoski, D. et al. (2017). The bioink: A comprehensive review on bioprintable materials. Biotechnol Adv 35, 217-239. doi:10.1016/j.biotechadv.2016.12.006
Hughes, C. S., Postovit, L. M. and Lajoie, G. A. (2010). Matrigel: A complex protein mixture required for optimal growth of cell culture. Proteomics 10, 1886-1890. doi:10.1002/pmic.200900758
Huh, D., Matthews, B. D., Mammoto, A. et al. (2010). Reconstituting organ-level lung functions on a chip. Science 328, 1662-1668. doi:10.1126/science.1188302
Kean, T. J. and Thanou, M. (2019). Utility of chitosan for 3D printing and bioprinting. In G. Crini and E. Lichtfouse (eds.), Sustainable Agriculture Reviews 35 (271-292). Cham, Switzerland: Springer. doi:10.1007/978-3-030-16538-3_6
Kleinman, H. K. (2001). Preparation of basement membrane components from EHS tumors. Curr Protoc Cell Biol Chapter 10, Unit 10 12. doi:10.1002/0471143030.cb1002s00
Ku, J., Seonwoo, H., Park, S. et al. (2020). Cell-laden thermosensitive chitosan hydrogel bioinks for 3D bioprinting applications. Appl Sci 10, 2455. doi:10.3390/app10072455
Langer, E. M., Allen-Petersen, B. L., King, S. M. et al. (2019). Modeling tumor phenotypes in vitro with three-dimensional bioprinting. Cell Rep 26, 608-623 e606. doi:10.1016/j.celrep.2018.12.090
Lee, A., Hudson, A. R., Shiwarski, D. J. et al. (2019). 3D bioprinting of collagen to rebuild components of the human heart. Science 365, 482-487. doi:10.1126/science.aav9051
Li, X., Liu, B., Pei, B. et al. (2020). Inkjet bioprinting of biomaterials. Chem Rev 120, 10793-10833. doi:10.1021/acs.chemrev.0c00008
Liu, T., Delavaux, C. and Zhang, Y. S. (2019). 3D bioprinting for oncology applications. J 3D Print Med 3, 55-58. doi:10.2217/3dp-2019-0004
Lopez-Marcial, G. R., Zeng, A. Y., Osuna, C. et al. (2018). Agarose-based hydrogels as suitable bioprinting materials for tissue engineering. ACS Biomater Sci Eng 4, 3610-3616. doi:10.1021/acsbiomaterials.8b00903
Ma, X., Qu, X., Zhu, W. et al. (2016). Deterministically patterned biomimetic human iPSC-derived hepatic model via rapid 3D bioprinting. Proc Natl Acad Sci U S A 113, 2206-2211. doi:10.1073/pnas.1524510113
Madden, L. R., Nguyen, T. V., Garcia-Mojica, S. et al. (2018). Bioprinted 3D primary human intestinal tissues model aspects of native physiology and ADME/Tox functions. iScience 2, 156-167. doi:10.1016/j.isci.2018.03.015
Marigliani, B., Balottin, L. B. L. and Augusto, E. F. P. (2019). Adaptation of mammalian cells to chemically defined media. Curr Protoc Toxicol 82, e88. doi:10.1002/cptx.88
Matai, I., Kaur, G., Seyedsalehi, A. et al. (2020). Progress in 3D bioprinting technology for tissue/organ regenerative engineering. Biomaterials 226, 119536. doi:10.1016/j.biomaterials.2019.119536
Matsuoka, Y., Lamirande, E. W. and Subbarao, K. (2009). The mouse model for influenza. Curr Protoc Microbiol Chapter 15, Unit 15G 13. doi:10.1002/9780471729259.mc15g03s13
Mendes, B. B., Gomez-Florit, M., Hamilton, A. G. et al. (2019). Human platelet lysate-based nanocomposite bioink for bioprinting hierarchical fibrillar structures. Biofabrication 12, 015012. doi:10.1088/1758-5090/ab33e8
Mondal, A., Gebeyehu, A., Miranda, M. et al. (2019). Characterization and printability of sodium alginate – Gelatin hydrogel for bioprinting NSCLC co-culture. Sci Rep 9, 19914. doi:10.1038/s41598-019-55034-9
Monferrer, E., Martin-Vano, S., Carretero, A. et al. (2020). A three-dimensional bioprinted model to evaluate the effect of stiffness on neuroblastoma cell cluster dynamics and behavior. Sci Rep 10, 6370. doi:10.1038/s41598-020-62986-w
Mota, C., Camarero-Espinosa, S., Baker, M. B. et al. (2020). Bioprinting: From tissue and organ development to in vitro models. Chem Rev 120, 10547-10607. doi:10.1021/acs.chemrev.9b00789
Ng, W. L., Wang, S., Yeong, W. Y. et al. (2016). Skin bioprinting: Impending reality or fantasy? Trends Biotechnol 34, 689-699. doi:10.1016/j.tibtech.2016.04.006
Nguyen, D. G., Funk, J., Robbins, J. B. et al. (2016). Bioprinted 3D primary liver tissues allow assessment of organ-level response to clinical drug induced toxicity in vitro. PLoS One 11, e0158674. doi:10.1371/journal.pone.0158674
Nguyen, D. G. and Pentoney, S. L., Jr. (2017). Bioprinted three dimensional human tissues for toxicology and disease modeling. Drug Discov Today Technol 23, 37-44. doi:10.1016/j.ddtec.2017.03.001
Nichol, J. W., Koshy, S. T., Bae, H. et al. (2010). Cell-laden microengineered gelatin methacrylate hydrogels. Biomaterials 31, 5536-5544. doi:10.1016/j.biomaterials.2010.03.064
Nielsen, O. B. and Hawkes, P. W. (2019). Fetal bovine serum and the slaughter of pregnant cows: Animal welfare and ethics. Bioprocess J 18. doi:10.12665/J18OA.Hawkes
Noor, N., Shapira, A., Edri, R. et al. (2019). 3D printing of personalized thick and perfusable cardiac patches and hearts. Adv Sci (Weinh) 6, 1900344. doi:10.1002/advs.201900344
Osidak, E. O., Kozhukhov, V. I., Osidak, M. S. et al. (2020). Collagen as bioink for bioprinting: A comprehensive review. Int J Bioprint 66, 270.
Oztan, Y. C., Nawafleh, N., Zhou, Y. et al. (2020). Recent advances on utilization of bioprinting for tumor modeling. Bioprinting 18, e00079. doi:10.1016/j.bprint.2020.e00079
Pons, M., Nagel, G., Zeyn, Y. et al. (2019). Human platelet lysate as validated replacement for animal serum to assess chemosensitivity. ALTEX 36, 277-288. doi:10.14573/altex.1809211
Psychogios, N., Hau, D. D., Peng, J. et al. (2011). The human serum metabolome. PLoS One 6, e16957. doi:10.1371/journal.pone.0016957
Puck, T. T., Cieciura, S. J. and Robinson, A. (1958). Genetics of somatic mammalian cells. III. Long-term cultivation of euploid cells from human and animal subjects. J Exp Med 108, 945-956. doi:10.1084/jem.108.6.945
Radigan, K. A., Misharin, A. V., Chi, M. et al. (2015). Modeling human influenza infection in the laboratory. Infect Drug Resist 8, 311-320. doi:10.2147/IDR.S58551
Rivero, S., Garcíaa, M. A. and Pinottiab, A. (2010). Crosslinking capacity of tannic acid in plasticized chitosan films. Carbohydr Polym 82, 270. doi:10.1016/j.carbpol.2010.04.048
Sanchez-Romero, N., Schophuizen, C. M., Gimenez, I. et al. (2016). In vitro systems to study nephropharmacology: 2D versus 3D models. Eur J Pharmacol 790, 36-45. doi:10.1016/j.ejphar.2016.07.010
Scherzer, M. T., Waigel, S., Donninger, H. et al. (2015). Fibroblast-derived extracellular matrices: An alternative cell culture system that increases metastatic cellular properties. PLoS One 10, e0138065. doi:10.1371/journal.pone.0138065
Schiele, N. R., Corr, D. T., Huang, Y. et al. (2010). Laser-based direct-write techniques for cell printing. Biofabrication 2, 032001. doi:10.1088/1758-5082/2/3/032001
Schiele, N. R., Chrisey, D. B. and Corr, D. T. (2011). Gelatin-based laser direct-write technique for the precise spatial patterning of cells. Tissue Eng Part C Methods 17, 289-298. doi:10.1089/ten.TEC.2010.0442
Schmidt, K., Berg, J., Roehrs, V. et al. (2020). 3D-bioprinted HepaRG cultures as a model for testing long term aflatoxin B1 toxicity in vitro. Toxicol Rep 7, 1578-1587. doi:10.1016/j.toxrep.2020.11.003
Schmidt, S. K., Schmid, R., Arkudas, A. et al. (2019). Tumor cells develop defined cellular phenotypes after 3D-bioprinting in different bioinks. Cells 8, 1295. doi:10.3390/cells8101295
Seok, J., Warren, H. S., Cuenca, A. G. et al. (2013). Genomic responses in mouse models poorly mimic human inflammatory diseases. Proc Natl Acad Sci U S A 110, 3507-3512. doi:10.1073/pnas.1222878110
Siramshetty, V. B., Nickel, J., Omieczynski, C. et al. (2016). WITHDRAWN – A resource for withdrawn and discontinued drugs. Nucleic Acids Res 44, D1080-1086. doi:10.1093/nar/gkv1192
Snyder, J. E., Hamid, Q., Wang, C. et al. (2011). Bioprinting cell-laden matrigel for radioprotection study of liver by pro-drug conversion in a dual-tissue microfluidic chip. Biofabrication 3, 034112. doi:10.1088/1758-5082/3/3/034112
Sriadibhatla, S., Yang, Z., Gebhart, C. et al. (2006). Transcriptional activation of gene expression by pluronic block copolymers in stably and transiently transfected cells. Mol Ther 13, 804-813. doi:10.1016/j.ymthe.2005.07.701
Su, K. and Wang, C. (2015). Recent advances in the use of gelatin in biomedical research. Biotechnol Lett 37, 2139-2145. doi:10.1007/s10529-015-1907-0
Sun, W., Starly, B., Daly, A. C. et al. (2020). The bioprinting roadmap. Biofabrication 12, 022002. doi:10.1088/1758-5090/ab5158
Swaminathan, S., Hamid, Q., Sun, W. et al. (2019). Bioprinting of 3D breast epithelial spheroids for human cancer models. Biofabrication 11, 025003. doi:10.1088/1758-5090/aafc49
Takao, K. and Miyakawa, T. (2015). Genomic responses in mouse models greatly mimic human inflammatory diseases. Proc Natl Acad Sci U S A 112, 1167-1172. doi:10.1073/pnas.1401965111
Toohey-Kurth, K., Sibley, S. D. and Goldberg, T. L. (2017). Metagenomic assessment of adventitious viruses in commercial bovine sera. Biologicals 47, 64-68. doi:10.1016/j.biologicals.2016.10.009
Tylek, T., Schilling, T., Schlegelmilch, K. et al. (2019). Platelet lysate outperforms FCS and human serum for co-culture of primary human macrophages and hMSCs. Sci Rep 9, 3533. doi:10.1038/s41598-019-40190-9
Usta, S. N., Scharer, C. D., Xu, J. et al. (2014). Chemically defined serum-free and xeno-free media for multiple cell lineages. Ann Transl Med 2, 97. doi:10.3978/j.issn.2305-5839.2014.09.05
van der Valk, J. and Gstraunthaler, G. (2017). Fetal bovine serum (FBS) – A pain in the dish? Altern Lab Anim 45, 329-332. doi:10.1177/026119291704500611
van der Valk, J., Bieback, K., Buta, C. et al. (2018). Fetal bovine serum (FBS): Past – Present – Future. ALTEX 35, 99-118. doi:10.14573/altex.1705101
Van Norman, G. A. (2019). Limitations of animal studies for predicting toxicity in clinical trials: Is it time to rethink our current approach? JACC Basic Transl Sci 4, 845-854. doi:10.1016/j.jacbts.2019.10.008
Vukicevic, S., Kleinman, H. K., Luyten, F. P. et al. (1992). Identification of multiple active growth factors in basement membrane Matrigel suggests caution in interpretation of cellular activity related to extracellular matrix components. Exp Cell Res 202, 1-8. doi:10.1016/0014-4827(92)90397-q
Wang, T., Lew, J., Premkumar, J. et al. (2017a). Production of recombinant collagen: State of the art and challenges. Eng Biol 1, 18-23. doi:10.1049/enb.2017.0003
Wang, X., Ao, Q., Tian, X. et al. (2017b). Gelatin-based hydrogels for organ 3D bioprinting. Polymers (Basel) 9, 401. doi:10.3390/polym9090401
Wang, Y., Shi, W., Kuss, M. et al. (2018). 3D bioprinting of breast cancer models for drug resistance study. ACS Biomater Sci Eng 4, 4401-4411. doi:doi/10.1021/acsbiomaterials.8b01277
Wei, Z., Liu, X., Ooka, M. et al. (2020). Two-dimensional cellular and three-dimensional bio-printed skin models to screen topical-use compounds for irritation potential. Front Bioeng Biotechnol 8, 109. doi:10.3389/fbioe.2020.00109
Weidner, C., Steinfath, M., Opitz, E. et al. (2016). Defining the optimal animal model for translational research using gene set enrichment analysis. EMBO Mol Med 8, 831-838. doi:10.15252/emmm.201506025
Weinhart, M., Hocke, A., Hippenstiel, S. et al. (2019). 3D organ model – Revolution in pharmacological research? Pharmacol Res 139, 446-451. doi:10.1016/j.phrs.2018.11.002
Wong, C. H., Siah, K. W. and Lo, A. W. (2019a). Estimation of clinical trial success rates and related parameters. Biostatistics 20, 273-286. doi:10.1093/biostatistics/kxx069
Wong, C. W., LeGrand, C. F., Kinnear, B. F. et al. (2019b). In vitro expansion of keratinocytes on human dermal fibroblast-derived matrix retains their stem-like characteristics. Sci Rep 9, 18561. doi:10.1038/s41598-019-54793-9
Wu, W., DeConinck, A. and Lewis, J. A. (2011). Omnidirectional printing of 3D microvascular networks. Adv Mater 23, H178-183. doi:10.1002/adma.201004625
Wu, Y., Zhang, Y., Yu, Y. and Ozbolat, I. T. (2020). 3D coaxial bioprinting of vasculature. Methods Mol Biol 2140, 171-181. doi:10.1007/978-1-0716-0520-2_11
Wu, Z. J., Su, X., Xu, Y. Y. et al. (2016). Bioprinting three-dimensional cell-laden tissue constructs with controllable degradation. Sci Rep 6, 24474. doi:10.1038/srep24474
Yang, G. H., Yeo, M., Koo, Y. W. et al. (2019). 4D bioprinting: Technological advances in biofabrication. Macromol Biosci 19, e1800441. doi:10.1002/mabi.201800441
Yao, T. and Asayama, Y. (2017). Animal-cell culture media: History, characteristics, and current issues. Reprod Med Biol 16, 99-117. doi:10.1002/rmb2.12024