Educational use of animals in Europe indicates reluctance to implement alternatives
Main Article Content
Abstract
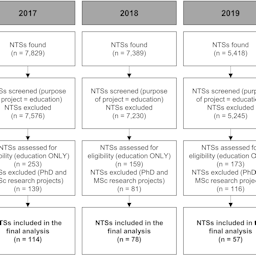
Animals have been considered an indispensable tool to teach about the functioning of living organisms, to obtain skills necessary for practicing human and veterinary medicine, as well as for acquiring skills for caring for and conducting experiments on animals in laboratories. However, the efficacy of this practice has been questioned in recent decades, and societal views have evolved to place a much stronger emphasis on animal welfare and ethics that needs to be reflected in our teaching and training practices. Currently, many alternatives to harmful animal use are available, and it is not clear why thousands of animals continue to be used every year for educational and training purposes. Therefore, this study aimed to identify reasons for the lack of uptake of non-harmful educational and training methods by analyzing recently published non-technical summaries in the EU and EEA Member States and to provide examples of alternatives for specific learning objectives. Results from non-technical summaries from 18 countries spanning the most recent years (2017-2019) revealed that the two main perceived reasons for continued animal use are: 1) the necessity to use a living animal for “proper” learning and 2) the lack of an adequate alternative. We argue that these reasons often do not reflect reality. In conclusion, we consider it is necessary to place a stronger emphasis on engagement with ethical questions that underlie the use of animals and careful consideration of how the learning objectives could be achieved through non-harmful alternatives.
Article Details

This work is licensed under a Creative Commons Attribution 4.0 International License.
Articles are distributed under the terms of the Creative Commons Attribution 4.0 International license (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution and reproduction in any medium, provided the original work is appropriately cited (CC-BY). Copyright on any article in ALTEX is retained by the author(s).
Abi-Rafeh, J., Zammit, D., Jaberi, M. M. et al. (2019). Nonbiological microsurgery simulators in plastic surgery training: A systematic review. Plast Reconstr Surg 144, 496e-507e. doi:10.1097/PRS.0000000000005990
Aboud, E., Suarez, C. E., Al-Mefty, O. et al. (2004). New alternative to animal models for surgical training. Altern Lab Anim 32, Suppl 1B, 501-507. doi:10.1177/026119290403201s80
Aboud, E. T., Aboud, G. and Aboud, T. (2015). “Live cadavers” for practicing airway management. Mil Med 180, Suppl 3, 165-170. doi:10.7205/MILMED-D-14-00396
Adams, C. M., Nigrovic, L. E., Hayes, G. et al. (2018). Teaching incision and drainage: Perceived educational value of abscess models. Pediatr Emerg Care 34, 174-178. doi:10.1097/PEC.0000000000001240
Akbarsha, M. A. (2007). Movement to curtail animal dissections in zoology curriculum: Review of the Indian experience. ALTEX 24, 163-166. doi:10.14573/altex.2007.3.163
Akbarsha, M. A., Zeeshan, M. and Meenakumari, K. J. (2013). Alternatives to animals in education, research, and risk assessment: An overview with special reference to Indian context. ALTEX Proc 2, 5-19. https://proceedings.altex.org/data/2013-01/rISC_001_Akbarsha2.pdf
Al-Elq, A. H. (2010). Simulation-based medical teaching and learning. J Family Community Med 17, 35-40. doi:10.4103/1319-1683.68787
Arluke, A. and Hafferty, F. (1996). From apprehension to fascination with “dog lab”: The use of absolutions by medical students. J Contemp Ethnogr 25, 201-225. doi:10.1177/089124196025002002
Atesok, K., Satava, R. M., Marsh, J. L. et al. (2017). Measuring surgical skills in simulation-based training. J Am Acad Orthop Surg 25, 665-672. doi:10.5435/JAAOS-D-16-00253
Aydin, A., Ahmed, K., Van Hemelrijck, M. et al. (2020). LBA01-05 simulation in urological training and education (SIMULATE): An international randomised controlled clinical and educational trial to determine the effect of simulation-based surgical training. J Urol 203, e1021-e1021. doi:10.1097/JU.0000000000000946.05
Baillie, S., Crossan, A., Brewster, S. A. et al. (2005a). Validation of a bovine rectal palpation simulator for training veterinary students. Stud Health Technol Inform 111, 33-36. http://eprints.gla.ac.uk/3729/
Baillie, S., Mellor, D. J., Brewster, S. A. et al. (2005b). Integrating a bovine rectal palpation simulator into an undergraduate veterinary curriculum. J Vet Med Educ 32, 79-85. doi:10.3138/jvme.32.1.79
Baillie, S., Crossan, A., Brewster, S. A. et al. (2010). Evaluating an automated haptic simulator designed for veterinary students to learn bovine rectal palpation. Simul Healthc 5, 261-266. doi:10.1097/SIH.0b013e3181e369bf
Balls, M. (2018). Replacing animal use in education and training. Altern Lab Anim 46, 107-108. doi:10.1177/026119291804600303
Balluch, M. (2006). Animals have a right to life. ALTEX 23, 281-293. https://www.altex.org/index.php/altex/article/view/804
Becker, G. J. (2007). Simulation and the coming transformation of medical education and training. Radiology 245, 7-9. doi:10.1148/radiol.2451070674
Bishop, L. J. and Nolen, A. L. (2001). Animals in research and education: Ethical issues. Kennedy Inst Ethics J 11, 91-112. doi:10.1353/ken.2001.0006
Bradley, P. (2006). The history of simulation in medical education and possible future directions. Med Educ 40, 254-262. doi:10.1111/j.1365-2929.2006.02394.x
Cagiltay, N. E., Ozcelik, E., Isikay, I. et al. (2019). The effect of training, used-hand, and experience on endoscopic surgery skills in an educational computer-based simulation environment (ECE) for endoneurosurgery training. Surg Innov 26, 725-737. doi:10.1177/1553350619861563
Can, A., Dao, D. T., Terrillion, C. E. et al. (2012). The tail suspension test. JoVE e3769. doi:10.3791/3769
Capaldo, T. (2004). The psychological effects on students of using animals in ways that they see as ethically, morally or religiously wrong. Altern Lab Anim 32, Suppl 1B, 525-531. doi:10.1177/026119290403201s85
Cingi, C. C., Baser, D. F., Karafakioglu, Y. S. et al. (2012). Stress response in dairy cows related to rectal examination. Acta Scientiae Veterinariae 40, 1053. https://www.redalyc.org/pdf/2890/289023557008.pdf
Clevenger, J. and Kass, P. H. (2003). Determinants of adoption and euthanasia of shelter dogs spayed or neutered in the University of California veterinary student surgery program compared to other shelter dogs. J Vet Med Educ 30, 372-378. doi:10.3138/jvme.30.4.372
Coombs, C. M., Shields, R. Y., Hunt, E. A. et al. (2017). Design, implementation, and evaluation of a simulation-based clinical correlation curriculum as an adjunctive pedagogy in an anatomy course. Acad Med 92, 494-500. doi:10.1097/ACM.0000000000001387
Crawford, S. B., Huque, Y. I., Austin, D. E. et al. (2019). Development and review of the chest tube high-feedback educational simulation trainer (CHEST). Simul Healthc 14, 276-279. doi:10.1097/sih.0000000000000361
Crofts, J. F., Bartlett, C., Ellis, D. et al. (2006). Training for shoulder dystocia: A trial of simulation using low-fidelity and high-fidelity mannequins. Obstet Gynecol 108, 1477-1485. doi:10.1097/01.AOG.0000246801.45977.c8
da Silva, A. P. G., Rodriguez, J. E. R., de Oliveira, M. C. et al. (2019). The alternative model of silicone for experimental simulation of suture of living tissue in the teaching of surgical technique. Acta Cir Bras 34, e201900410. doi:10.1590/s0102-865020190040000010
Davies, J., Khatib, M. and Bello, F. (2013). Open surgical simulation: A review. J Surg Educ 70, 618-627. doi:10.1016/j.jsurg.2013.04.007
de Souza, M. C. C. M. I. and Matera, J. M. (2015). Bleeding simulation in embalmed cadavers: Bridging the gap between simulation and live surgery. ALTEX 32, 59-63. doi:10.14573/altex.1407311
De Villiers, R. and Monk, M. (2005). The first cut is the deepest: Reflections on the state of animal dissection in biology education. J Curric Stud 37, 583-600. doi:10.1080/00220270500041523
Deonarain, A. R., Harrison, R. V., Gordon, K. A. et al. (2020). Live porcine model for surgical training in tracheostomy and open‐airway surgery. Laryngoscope 130, 2063-2068. doi:10.1002/lary.28309
Dewhurst, D. (2008). Is it possible to meet the learning objectives of undergraduate pharmacology classes with non-animal models? AATEX 14, 207-212. http://www.asas.or.jp/jsaae_old/aatex/Vol12S.html
Draycott, T., Sibanda, T., Owen, L. et al. (2006). Does training in obstetric emergencies improve neonatal outcome? BJOG 113, 177-182. doi:10.1111/j.1471-0528.2006.00800.x
Duhem, H., Viglino, D., Bellier, A. et al. (2019). Cadaver models for cardiac arrest: A systematic review and perspectives. Resuscitation 143, 68-76. doi:10.1016/j.resuscitation.2019.08.009
Durand, M. d. T., Restini, C. B. A., Wolff, A. C. D. et al. (2019). Students’ perception of animal or virtual laboratory in physiology practical classes in PBL medical hybrid curriculum. Adv Physiol Educ 43, 451-457. doi:10.1152/advan.00005.2019
Engel, R. M., Silver, C. C., Veeder, C. L. et al. (2020). Cognitive dissonance in laboratory animal medicine and implications for animal welfare. J Am Assoc Lab Anim Sci 59, 132-138. doi:10.30802/AALAS-JAALAS-19-000073
EC – European Commission (2009). Final report of the expert working group on severity classification of scientific procedures performed on animals. https://ec.europa.eu/environment/archives/lab_animals/ewg_en.htm
EC (2013). Working document on Non-Technical Project summaries. https://ec.europa.eu/environment/chemicals/lab_animals/pdf/Recommendations%20for%20NTS.pdf
EC (2020). 2019 Report on the statistics on the use of animals for scientific purposes in the Member States of the European Union in 2015-2017. Report from the Commission to the European Parliament and the Council. EC.
Feins, R. H., Burkhart, H. M., Conte, J. V. et al. (2017). Simulation-based training in cardiac surgery. Ann Thorac Surg 103, 312-321. doi:10.1016/j.athoracsur.2016.06.062
Fowler, H. S. and Brosius, E. J. (1968). A research study on the values gained from dissection of animals in secondary school biology. Sci Educ 52, 55-57. doi:10.1002/sce.3730520114
Gala, S. G. and Crandall, M. L. (2019). Global collaboration to modernize advanced trauma life support training. J Surg Educ 76, 487-496. doi:10.1016/j.jsurg.2018.08.011
Garcia, D. F. V., Domingues, C. A., Collet e Silva, F. S. et al. (2019). Efficacy of a novel surgical manikin for simulating emergency surgical procedures. Am Surg 85, 1318-1326. http://observatorio.fm.usp.br/handle/OPI/34256
Gelberg, S. and Gelberg, H. (2005). Stress management interventions for veterinary students. J Vet Med Educ 32, 173-181. doi:10.3138/jvme.32.2.173
Giese, H., Hilke, J., Gundelach, Y. et al. (2015). Validation of a bovine vascular access model for teaching students a technique for placing catheter in the auricular vein of cattle. InVeST Conference 2015, https://bit.ly/2RgPbhk
Giese, H., Dilly, M., Gundelach, Y. et al. (2018). Influence of transrectal palpation training on cortisol levels and heart rate variability in cows. Theriogenology 119, 238-244. doi:10.1016/j.theriogenology.2018.07.016
Giménez, M. E., Garcia Vazquez, A., Davrieux, C. F. et al. (2020). Image-guided surgical training in percutaneous hepatobiliary procedures: Development of a realistic and meaningful bile duct dilatation porcine model. J Laparoendoscopic Adv Surg Tech A, online ahead of print. doi:10.1089/lap.2020.0680
Graham, J., Alloway, T. and Krames, L. (1994). Sniffy, the virtual rat: Simulated operant conditioning. Behav Res Methods Instrum Comput 26, 134-141. doi:10.3758/BF03204606
Grant, J. S., Moss, J., Epps, C. et al. (2010). Using video-facilitated feedback to improve student performance following high-fidelity simulation. Clin Simul Nurs 6, e177-e184. doi:10.1016/j.ecns.2009.09.001
Grevemeyer, B. and Knight, A. (2018). The development of a clinical skills laboratory at Ross University School of Veterinary Medicine. Altern Lab Anim 46, 177-183. doi:10.1177/026119291804600305
Griswold, S., Ponnuru, S., Nishisaki, A. et al. (2012). The emerging role of simulation education to achieve patient safety: Translating deliberate practice and debriefing to save lives. Pediatr Clin North Am 59, 1329-1340. doi:10.1016/j.pcl.2012.09.004
Guedes, H. G., Câmara Costa Ferreira, Z. M., Ribeiro de Sousa Leão, L. et al. (2019). Virtual reality simulator versus box-trainer to teach minimally invasive procedures: A meta-analysis. Int J Surg 61, 60-68. doi:10.1016/j.ijsu.2018.12.001
Hall, A. B., Riojas, R. and Sharon, D. (2014). Comparison of self-efficacy and its improvement after artificial simulator or live animal model emergency procedure training. Mil Med 179, 320-323. doi:10.7205/milmed-d-12-00446
Hansen, L. A. (2014). Animal laboratories are not needed to train medical students. J Surg Educ 71, 454. doi:10.1016/j.jsurg.2014.02.001
Hardman, J. G. and Ross, J. J. (2006). Modelling: A core technique in anaesthesia and critical care research. Br J Anaesth 97, 589-592. doi:10.1093/bja/ael272
Hart, L. A., Wood, M. W. and Hart, B. L. (2008). Why Dissection? Animal Use in Education. Westport, CT, USA: Greenwood Press.
Hellyer, P., Frederick, C., Lacy, M. et al. (1999). Attitudes of veterinary medical students, house officers, clinical faculty, and staff toward pain management in animals. J Am Vet Med Assoc 214, 238-244. https://europepmc.org/article/med/9926017
Howe, L. M. and Slater, M. R. (1997). Student assessment of the educational benefits of a prepubertal gonadectomy program (preliminary findings). J Vet Med Educ 24, 12-17. https://bit.ly/3xH2g4c
Ille, N., Aurich, C. and Aurich, J. (2016). Physiological stress responses of mares to gynecologic examination in veterinary medicine. J Equine Vet Sci 43, 6-11. doi:10.1016/j.jevs.2016.04.010
Jaskowski, J. M., Sobolewski, J., Wieczorkiewicz, M. et al. (2020). Modern techniques of teaching bovine rectal palpation: Opportunities, benefits and disadvantages of new educational devices. Med Weter 76, 5-10. doi:10.21521/mw.6324
Jensen, K. K. (2017). How should death be taken into account in welfare assessments? J Agric Environ Ethics 30, 615-623. doi:10.1007/s10806-017-9688-1
Jukes, N. (2004). Are animals necessary in biological education? Altern Lab Anim 32, Suppl 1B, 753-754. doi:10.1177/026119290403201s124
Kaldewaij, F. (2006). Animals and the harm of death. In M. Kaiser and M. E. Lien (eds.), Ethics and the Politics of Food. Oslo, Norway: Congress of the European Society for Agricultural and Food Ethics.
Kinnison, T., Forrest, N. D., Frean, S. P. et al. (2009). Teaching bovine abdominal anatomy: Use of a haptic simulator. Anat Sci Educ 2, 280-285. doi:10.1002/ase.109
Knight, A. (2007). The effectiveness of humane teaching methods in veterinary education. ALTEX 24, 91-109. doi:10.14573/altex.2007.2.91
Knight, A. (2011). The Costs and Benefits of Animal Experiments. The Palgrave Macmillan Animal Ethics Series. London, UK: Palgrave Macmillan UK.
Knight, A. (2012). The potential of humane teaching methods within veterinary and other biomedical education. ALTEX Proc 1, 365-375. doi:10.14573/altex.2007.2.91
Kovatch, K. J., Powell, A. R., Green, K. et al. (2020). Development and multidisciplinary preliminary validation of a 3-dimensional-printed pediatric airway model for emergency airway front-of-neck access procedures. Anesth Analg 130, 445-451. doi:10.1213/ane.0000000000003774
Kuhse, H. and Singer, P. (1998). A Companion to Bioethics. Malden, MA, USA: Blackwell Publishing.
Labrague, L. J., McEnroe-Petitte, D. M., Bowling, A. M. et al. (2019). High-fidelity simulation and nursing students’ anxiety and self-confidence: A systematic review. Nurs Forum 54, 358-368. doi:10.1111/nuf.12337
Lewis, J. L. (2015). A comparison between two different activities for teaching learning principles: Virtual animal labs versus human demonstrations. Scholarsh Teach Learn Psychol 1, 182. doi:10.1037/stl0000013
Marker, S., Mohr, M. and Østergaard, D. (2019). Simulation-based training of junior doctors in handling critically ill patients facilitates the transition to clinical practice: An interview study. BMC Med Educ 19, 11. doi:10.1186/s12909-018-1447-0
Martinsen, S. and Jukes, N. (2005). Towards a humane veterinary education. J Vet Med Educ 32, 454-460. doi:10.3138/jvme.32.4.454
McLaughlin, C., Barry, W., Barin, E. et al. (2019). Multidisciplinary simulation-based team training for trauma resuscitation: A scoping review. J Surg Educ 76, 1669-1680. doi:10.1016/j.jsurg.2019.05.002
Meurling, L., Hedman, L., Sandahl, C. et al. (2013). Systematic simulation-based team training in a Swedish intensive care unit: A diverse response among critical care professions. BMJ Qual Saf 22, 485-494. doi:10.1136/bmjqs-2012-000994
Moher, D., Liberati, A., Tetzlaff, J. et al. (2009). Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. PLoS Med 6, e1000097. doi:10.1371/journal.pmed.1000097
Müller, L. R., Tipold, A., Ehlers, J. P. et al. (2019). TiHoVideos: Veterinary students’ utilization of instructional videos on clinical skills. BMC Vet Res 15, 326. doi:10.1186/s12917-019-2079-2
Nakao, T., Sato, T., Moriyoshi, M. et al. (1994). Plasma cortisol response in dairy cows to vaginoscopy, genital palpation per rectum and artificial insemination. J Vet Med A Physiol Pathol Clin Med 41, 16-21. doi:10.1111/j.1439-0442.1994.tb00060.x
Oakley, J. (2012). Science teachers and the dissection debate: Perspectives on animal dissection and alternatives. Int J Environ Sci Educ 7, 253-267. doi:10.1080/21548455.2016.1254358
Oakley, J. (2013). “I didn’t feel right about animal dissection”. Dissection objectors share their science class experiences. Soc Anim 21, 360-378. doi:10.1163/15685306-12341267
Oberoi, G., Eberspächer-Schweda, M. C., Hatamikia, S. et al. (2020). 3D printed biomimetic rabbit airway simulation model for nasotracheal intubation training. Front Vet Sci 7, 587524. doi:10.3389/fvets.2020.587524
Okhovat, S., Milner, T. D., Clement, W. A. et al. (2020). Validation of animal models for simulation training in pediatric laryngotracheal reconstruction. Ann Otol Rhinol Laryngol 129, 46-54. doi:10.1177/0003489419870820
Patronek, G. J. and Rauch, A. (2007). Systematic review of comparative studies examining alternatives to the harmful use of animals in biomedical education. J Am Vet Med Assoc 230, 37-43. doi:10.2460/javma.230.1.37
Paul, E. S. and Podberscek, A. L. (2000). Veterinary education and students’ attitudes towards animal welfare. Vet Rec 146, 269-272. doi:10.1136/vr.146.10.269
Pawlowski, J. B., Feinstein, D. M. and Gala, S. G. (2018). Developments in the transition from animal use to simulation-based biomedical education. Simul Healthc 13, 420-426. doi:10.1097/sih.0000000000000310
Pereira, G. D., Dieguez, J., Demirbas, Y. S. et al. (2017). Alternatives to animal use in veterinary education: A growing debate. Ankara Universitesi Veteriner Fakultesi Dergisi 64, 235-239. doi:10.1501/Vetfak_0000002804
Pirrone, F., Mariti, C., Gazzano, A. et al. (2019). Attitudes toward animals and their welfare among Italian veterinary students. Vet Sci 6, 19. doi:10.3390/vetsci6010019
Quilici, A. P., Bicudo, A. M., Gianotto-Oliveira, R. et al. (2015). Faculty perceptions of simulation programs in healthcare education. Int J Med Educ 6, 166-171. doi:10.5116/ijme.5641.0dc7
Quiroga, M. d. M., Clarke, S. and Rajan, R. (2016). Online simulations to support the teaching of physiology. FASEB J 30, 553.521. doi:10.1096/fasebj.30.1_supplement.553.21
Rathod, S., Ghoderao, D., Kolte, V. et al. (2019). Simulation-based surgical skill training in internship program. SRM J Res Dent Sci 10, 135-138. doi:10.4103/srmjrds.srmjrds_45_19
Rezende-Filho, F. M., da Fonseca, L. J. S., Nunes-Souza, V. et al. (2014). A student-centered approach for developing active learning: The construction of physical models as a teaching tool in medical physiology. BMC Med Educ 14, 189. doi:10.1186/1472-6920-14-189
Richardson, E. F., Gregory, C. R. and Sucre, E. (1994). Enhancement of the surgical education of fourth year veterinary students by participation in juvenile ovariohysterectomy and castration program. Vet Surg 23, 415. doi:10.1111/j.1532-950X.1994.tb00500.x
Rosen, M. A., Weaver, S. J., Lazzara, E. H. et al. (2010). Tools for evaluating team performance in simulation-based training. J Emerg Trauma Shock 3, 353-359. doi:10.4103/0974-2700.70746
Rubeis, G. and Steger, F. (2018). Is live-tissue training ethically justified? An evidence-based ethical analysis. Altern Lab Anim 46, 65-71. doi:10.1177/026119291804600206
Russell, W. M. S. and Burch, R. L. (1959). The Principles of Humane Experimental Technique. London, UK: Methuen.
Salas, E., Rosen, M. A., Held, J. D. et al. (2009). Performance measurement in simulation-based training: A review and best practices. Simul Gaming 40, 328-376. doi:10.1177/1046878108326734
Self, D. J., Schrader, D. E., Baldwin, J. D. et al. (1991). Study of the influence of veterinary medical education on the moral development of veterinary students. J Am Vet Med Assoc 198, 782-787. https://europepmc.org/article/med/1953847
Šilar, J., Polák, D., Mládek, A. et al. (2019). Development of in-browser simulators for medical education: Introduction of a novel software toolchain. J Med Internet Res 21, e14160. doi:10.2196/14160
Silverplats, K., Jonsson, A. and Lundberg, L. (2016). A hybrid simulator model for the control of catastrophic external junctional haemorrhage in the military environment. Adv Simul 1, 5. doi:10.1186/s41077-016-0008-z
Strittmatter, S. (2017). Undervaluation of suffering of experimental animals in Germany. ALTEX 34, 435-438. https://www.altex.org/index.php/altex/article/view/39
Tanya, S. and Dubrowski, A. (2020). Development of a cost-effective pediatric intubation task trainer for rural medical education. Cureus 12, e6604. doi:10.7759/cureus.6604
Taylor, K., Rego, L. and Weber, T. (2018). Recommendations to improve the EU non-technical summaries of animal experiments. ALTEX 35, 193-210. doi:10.14573/altex.1708111
Tolbert, S. (2019). Queering dissection: “I wanted to bury its heart, at least”. In C. Taylor, C. Amade-Escote and A. Abbas (eds.), Gender in Learning and Teaching: Feminist Dialogues Across International Boundaries. London, UK: Routledge.
Ulmer, F., Lennertz, J., Greif, R. et al. (2020). Emergency front of neck access in children: A new learning approach in a rabbit model. Br J Anaesth 125, e61-e68. doi:10.1016/j.bja.2019.11.002
Valliyate, M., Robinson, N. G. and Goodman, J. R. (2012). Current concepts in simulation and other alternatives for veterinary education: A review. Vet Med (Praha) 57, 325-337. doi:10.17221/6261-vetmed
van Vollenhoven, E., Fletcher, L., Page, P. C. et al. (2017). Heart rate variability in healthy, adult pony mares during transrectal palpation of the reproductive tract by veterinary students. J Equine Vet Sci 58, 68-77. doi:10.1016/j.jevs.2017.08.013
Villanueva, C., Xiong, J. and Rajput, S. (2019). Simulation‐based surgical education in cardiothoracic training. ANZ J Surg doi:10.1111/ans.15593
Vogt, L., Duckwitz, V., Arlt, S. P. et al. (2019). Teaching small animal reproduction via virtual patients. Reprod Domest Anim 55, Suppl 2, 81-89. doi:10.1111/rda.13598
Waldau, P. (2007). Veterinary education as leader: Which alternatives? J Vet Med Educ 34, 605-614. doi:10.3138/jvme.34.5.605
Wijewickrema, S., Ma, X., Piromchai, P. et al. (2018). Providing automated real-time technical feedback for virtual reality based surgical training: Is the simpler the better? In C. Penstein Rosé, R. Martínez-Maldonado, H. U. Hoppe et al. (eds.), Artificial Intelligence in Education, Lecture Notes in Computer Science. Cham, Switzerland: Springer International Publishing.
Xiberta, P. and Boada, I. (2019). IVET, an interactive veterinary education tool. J Anim Sci 97, 932-944. doi:10.1093/jas/sky471
Yankelevitch-Yahav, R., Franko, M., Huly, A. et al. (2015). The forced swim test as a model of depressive-like behavior. J Vis Exp, e52587. doi:10.3791/52587
Yeates, J. W. (2010). Death is a welfare issue. J Agric Environ Ethics 23, 229-241. doi:10.1007/s10806-009-9199-9
Yong, J. A. A., Case, J. B., Kim, S. E. et al. (2019). Survey of instructor and student impressions of a high-fidelity model in canine ovariohysterectomy surgical training. Vet Surg 48, 975-984. doi:10.1111/vsu.13218
Zemanova, M. A. and Knight, A. (2021). The educational efficacy of humane teaching methods: A systematic review of the evidence. Animals 11, 114. doi:10.3390/ani11010114
Zuna, I. and Holt, A. (2017). ADAM, a hands-on patient simulator for teaching principles of drug disposition and compartmental pharmacokinetics. Br J Clin Pharmacol 83, 2426-2449. doi:10.1111/bcp.13357